There’s a lot to consider when choosing an insulin pump.
In this article we’ll cover what an insulin pump is, how they work, and the different brand options out there. I also have a helpful table at the end that compares the three most common brands available in the United States.
What is an insulin pump?
Insulin injections are necessary for people living with type 1 diabetes and people with type 2 diabetes whose pancreas don’t produce enough insulin. There are options for insulin delivery for these people including:
- Injection by insulin syringes
- Injection by insulin pens
- Insulin pump.

The first two options, which most people think of, is an injection of insulin under the skin with syringes or pen needles. The next option is insulin injections using an insulin pump. You may be wondering what an insulin pump is, but don’t worry we will try to answer all of your questions below. We are going to go into a little bit of detail about the way pumps work and the different types of insulin pumps on the market.
***This article is not intended to provide medical advice, diagnosis, opinion, treatment or services. This article and the links contained in it provide general information for educational purposes only. The information provided in this article is not a substitute for medical care, and should not be used in place of the advice of your physician or registered dietitian.
How does an insulin pump work?
An insulin pump infuses insulin under the skin, to help manage glucose levels by using bolus injections (when you eat carbohydrate or to correct a high blood sugar) and basal/continuous infusions every 3-5 minutes (to mimic the natural drip of insulin from a functioning pancreas.
In type 1 diabetes, the pancreas is no longer able to produce any insulin at all, so a basal injection or continuous drip is needed. Pumps infuse a basal dose of insulin every 3 to 5 minutes in an attempt to mimic pancreas activity in order to lower glucose in the blood stream. You can also program the insulin pump to inject a bolus dose (a larger dose) of insulin when necessary, like before eating or in times when blood sugar correction is necessary.
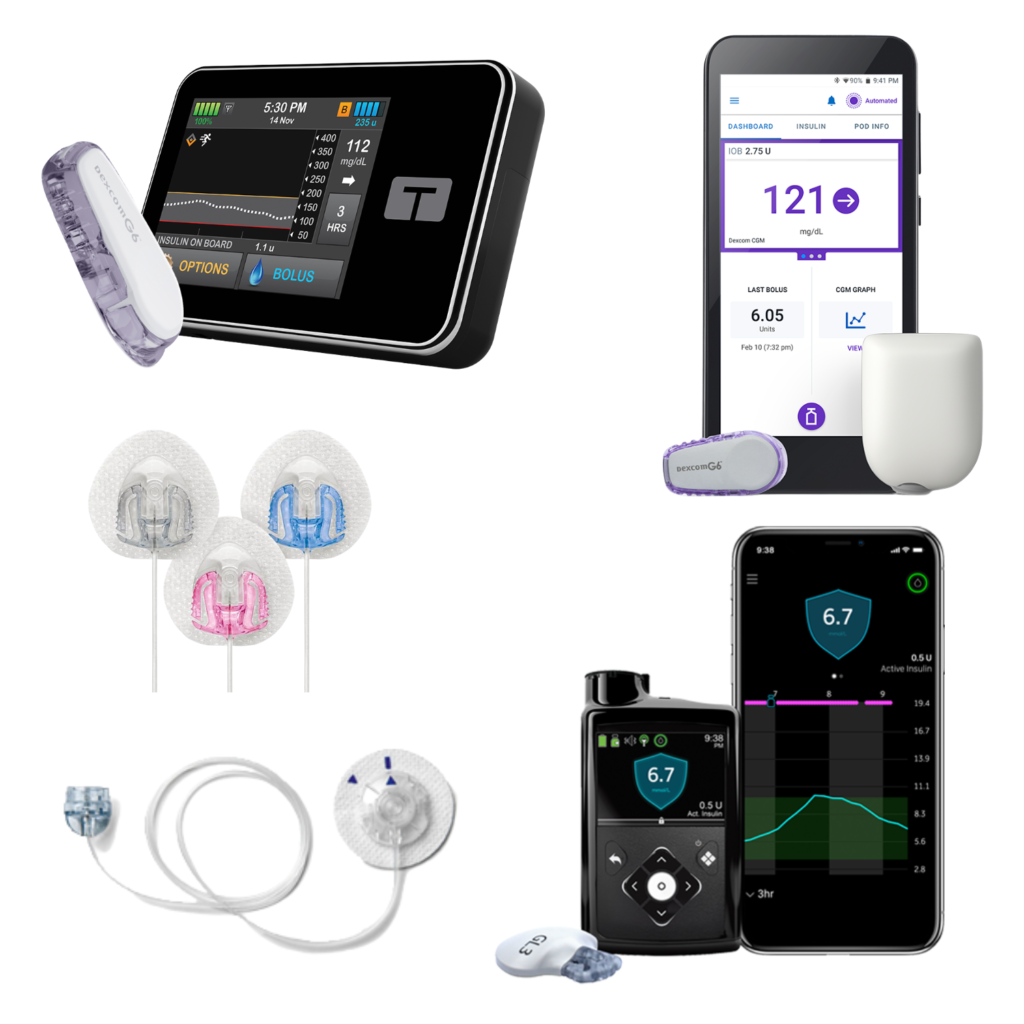
No single method or insulin regimen is a better option than the other. It is person-specific and one regimen might work better for you than others. Setting basal doses and bolus doses might change from day to day, and hour to hour and can be adjusted. Below we are going to talk about three different types of insulin pumps and how they compare to one another. The three pumps we are going to talk about are Tandem, Medtronic, and Omnipod. As always, speak to your doctor with any questions you may have.
Tandem
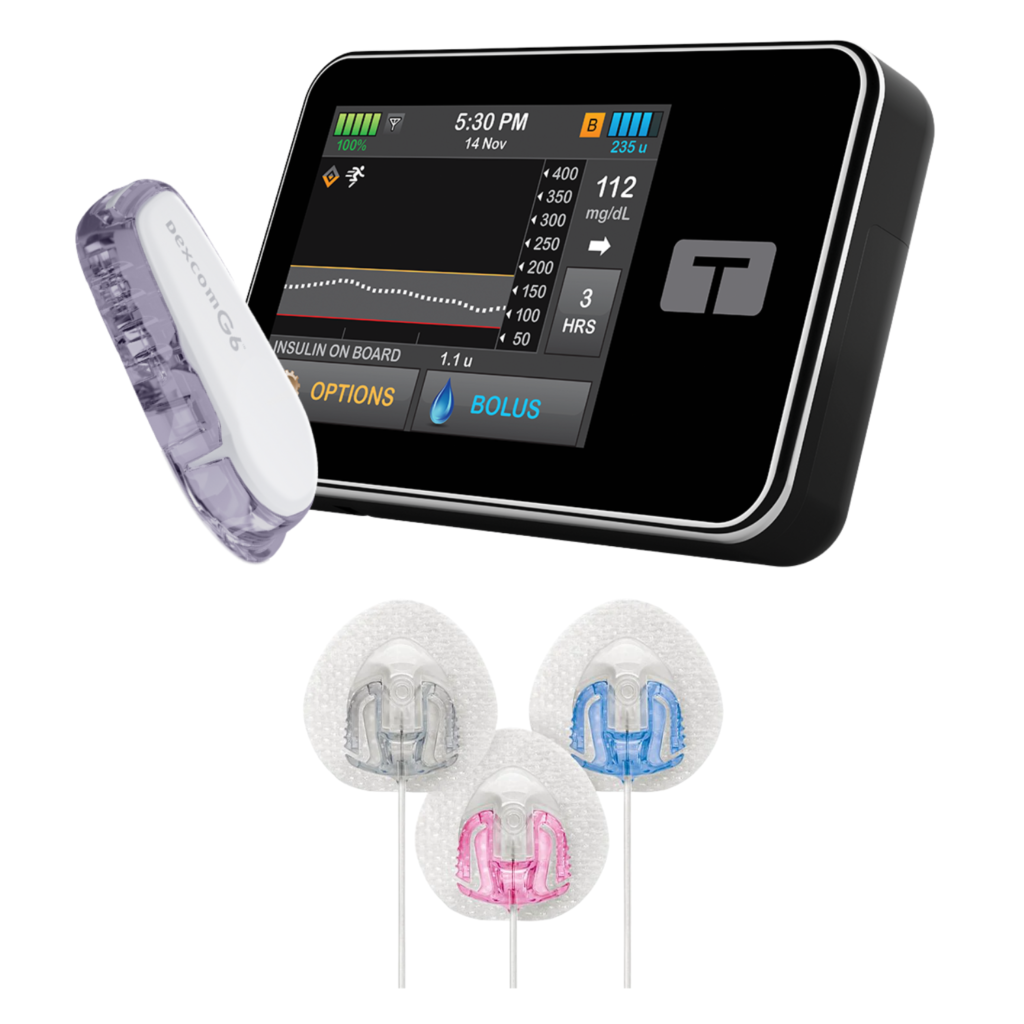
The first pump we are going to discuss is the Tandem Diabetes Care insulin pump. There are several previous Tandem models, but the most recent one is the T-slim X2 Pump. This model is a slim touchscreen device with a rechargeable battery and a 300-unit cartridge. A tube from the device to the cannula on the stomach is used to deliver insulin into the body.
The T-Slim has Control-IQ and Basal-IQ technology that works with the Dexcom G6 continuous glucose monitoring (CGM) system to help deliver insulin, predict glucose levels 30 minutes in advance, and prevent high and low glucose levels. This technology is a helpful tool used to successfully manage diabetes, but glucose levels should still be carefully monitored. The sleek touch screen makes it easy to observe the amount of insulin delivered and glucose history. Tandem also offers a t:connect mobile app that allows users to bolus directly from a compatible device and view pump data to help understand glucose levels and insulin deliveries.
Medtronic
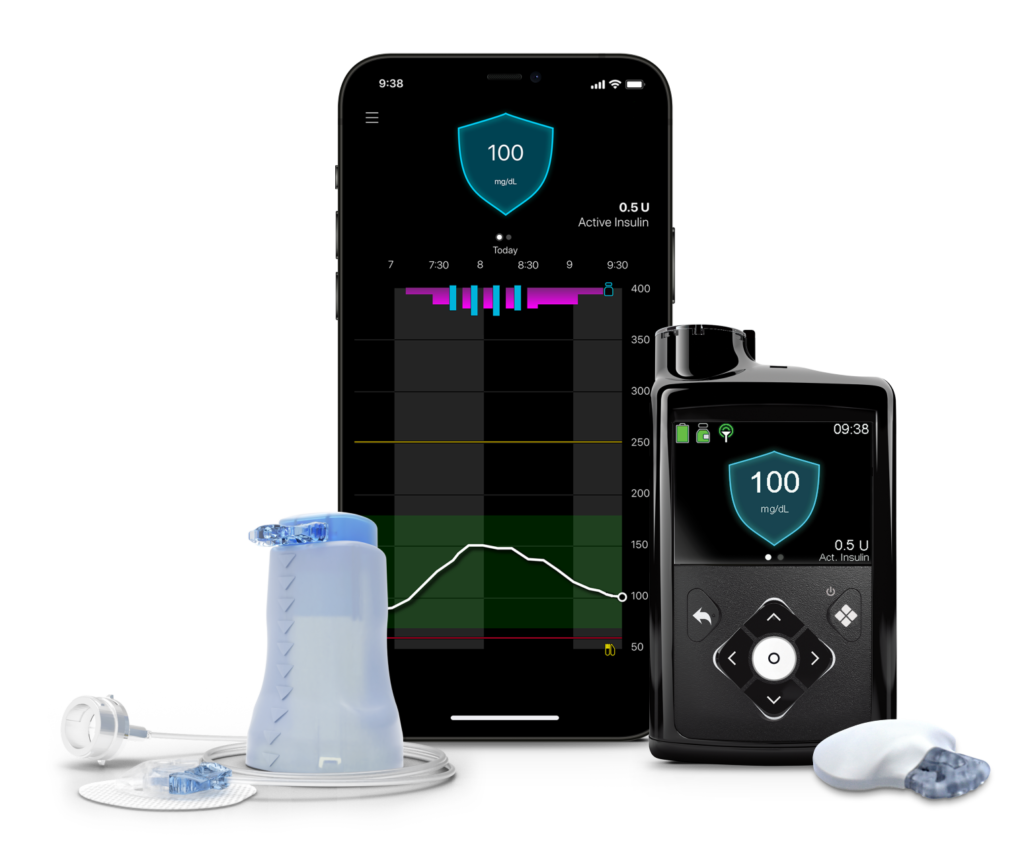
The Medtronic system we will discuss is the MiniMed™ 780G system. This system is for type 1 diabetes only, but there is a MiniMed 630G system for type 1 and type 2 diabetes. Like the Tandem model previously discussed, the Minimed also has tubing and a 300-unit reservoir. This tubing goes from the insulin pump to the insertion site on the abdomen and is changed every 2 to 3 days, and up to 7 days for the Medtronic Extend infusion set. Like the Tandem, MiniMed has a continuous glucose sensor called the Guardian™ 4 sensor.
This sensor is attached to the back of the upper arm and tests the blood glucose levels every 5 minutes. No calibrations are needed with SmartGuard™ technology. The blood glucose level is then sent wirelessly to the pump which will adjust background/basal insulin (that continuous drip I mentioned above) according to the glucose level. This SmartGuard technology will help prevent highs and lows of blood sugar.
Like the Tandem model previously discussed, the Minimed also has tubing and a 300-unit reservoir. This tubing goes from the insulin pump to the insertion site on the abdomen and is changed every 2 to 3 days, and up to 7 days for the Medtronic Extend infusion set. Like the Tandem, MiniMed has a continuous glucose sensor called the Guardian™ 4 sensor. This sensor is attached to the back of the upper arm and tests the blood glucose levels every 5 minutes. No calibrations are needed with SmartGuard™ technology. The blood glucose level is then sent wirelessly to the pump which will adjust background/basal insulin (that continuous drip I mentioned above) according to the glucose level. This SmartGuard technology will help prevent highs and lows of blood sugar.
Before meals, enter the amount of carbs in the meal and the pump will give a recommended amount of insulin for a bolus injection of insulin. If a meal dose is missed or miscalculated, Meal Detection™ technology automatically detects, adjusts, and corrects glucose levels every 5 minutes.
Again, this technology is helpful for controlling diabetes and glucose levels, but self-monitoring is also necessary. This can be achieved with the same Guardian sensor. The monitoring from the sensor can be sent right to your smartphone for easy monitoring. However, the current model does not offer users to deliver insulin through the smartphone app.
Omnipod

The last pump we will be discussing is the Omnipod 5. The Omnipod is the only pod injection system we will be discussing. This is a tubeless system with a pod holding 200 units of insulin. The small waterproof pod is placed on the abdomen or back of the arm and can be controlled by a separate Personal Diabetes Manager (PDM) that looks like a typical smartphone or on select android phones. Currently, the Omnipod 5 is not iOS compatible.
First, you have to fill a pod with insulin and attach it to the arm or abdomen. Filling the pod is much like filling the reservoirs from the previous two pumps discussed. In the simplest description, using a needle and syringe, insulin is drawn out of the vial and injected into the pod. The pod will last for 3 days (72 hours of insulin delivery) before needing to be changed out for a new pod.
Using the PDM or the smartphone app, you will program your basal rate in the PDM for a continuous infusion of insulin. The Omnipod 5 is the first and only insulin pump on the market that has an automated delivery system and is tubeless. Similar to the T-slim X2 Pump, the Omnipod 5 is integrated with the Dexcom G6 CGM to correct glucose levels.
However, this pump does not deliver auto-correction boluses to address high glucose levels, requiring users to self administer to correct highs. Just like the other pumps you are able to enter the information about meals and carbohydrates to begin a bolus injection of insulin. There is also a CalorieKing Database included on the PDM that has the carbohydrate count for many foods that will help adjust the bolus injection.
Insulin pump cost and overview
| Tandem/T-Slim | Medtronic/Minimed 770G System | Omnipod 5 | |
| Waterproof* | Yes | Yes | Yes |
| Battery | Rechargeable | 1 AA | Rechargeable |
| Out of Pocket Cost** | ~$4000 | ~$7300 | ~$300 (for 5 pods) |
| Insurance coverage | Covered under most insurances | Covered under most insurances | Covered under most insurances |
| Tubing | Yes | Yes | No |
| Units | 300-unit reservoir | 300-unit reservoir | 200-unit pod |
| Activity mode | Yes | Yes | Yes |
| Bolus Range | 0.05 to 25 units | 0.025 to 25 units | 0.05 to 30 units |
| Basal Range | 0.1 to 15 units/hr 0.001 unit increments | 0.025 to 35 units/hr 0.025 unit increments | 0 to 30 units/hr 0.05 unit increments |
| Monitoring technology | Yes with Dexcom | Yes with Medtronic Guardian Sensor 3 | Yes with Dexcom |
| Prediction Time | 30 minutes | 30 minutes | 60 minutes |
| Pump Controller | Pump controller & Smart phone (iOS & Android compatible) | Pump Controller | Pump controller & Smart phone (Android compatible for select models) |
| Automatic Correction Boluses | Yes | Yes | Yes |
| Age Range | 14 years or greater | 2 years or greater | 2 years or greater |
**Many will allow a payment plan for out of pocket cost
Pump supplies
The initial cost of an insulin pump can be quite large as seen above, but it’s also important to factor the monthly supply cost for infusion sets, cartridges and/or pods. Months supply costs can range from $300-$600 cash price. (This will change based on your level of insurance coverage.
Insulin pump Accessories
There’s also numerous ways to personalize your pump through fun adhesion tapes, cook covers/protectors, and carrying cases. A simple google search for “fun insulin pump accessories” will bring up a whole host of websites offering some great options!
Insulin pump accessories
There’s also numerous ways to personalize your pump through fun adhesion tapes, cook covers/protectors, and carrying cases. A simple google search for “fun insulin pump accessories” will bring up a whole host of websites offering some great options!
In summary, choosing to go on an insulin pump and subsequently which type of insulin pump is right for you is a very personal choice. Seek out support from loved ones and your health care professionals.
This post was originally published in November 2020, and was updated in January 2023 to reflect current technology.







2 Responses
There is a ton of useful info in here. I was recently diagnosed with type 2 diabetes and I was shocked when my nurse practitioner said that she was wanted to get me started on an insulin pump. My A1C was 8.8 and I had heard that insulin was very rarely used as an initial treatment for people who had an A1C of less than 9.0. She told me that there is a lot of new research suggesting that T2D patients who start insulin early (or at the time of diagnosis) are having better outcomes. I am definitely still in the process of getting used to this (it is a BIG change to have something connected to your body, and that’s in addition to the CGM). I guess I do feel somewhat better knowing that my blood sugar is being controlled automatically and that my NP can see all of my data that gets uploaded. I am nearly a month in and I have gained some weight (3.8 pounds) which is a little concerning although most of it came in the first two weeks. Something we are monitoring, though. Again, thank you for the information in this article and I am sure there may be others like myself who find themselves on insulin sooner rather than later after a new T2D diagnosis.
I’m so glad I found this blog post! I’ve been looking for information about diabetes insulin pumps for a while now. I’m currently using a Medtronic pump and I’m really happy with it. I’m looking into the