
In this article, we discuss what exactly “early diabetes feet” is, signs of diabetes feet, what to look out for, and how to take care of your feet.
Diabetes management requires you to be mindful of what you eat, take medicine, monitor your blood sugars, and visit the doctor. On top of all of that, foot health might not be top of mind, but ignoring early diabetes feet care can lead to serious consequences.
What is “diabetes feet”?
Diabetes feet refers to foot problems related to diabetes complications. Diabetes increases the risk of nerve damage and poor circulation. These can lead to slow wound healing, calluses, corns, bunions, cracked heels, ingrown toenails, infection, and blisters. Over time, it can also cause numbness or a tingly, “pins and needle” sensation. This can make detecting open sores, cuts, or other problems more difficult.
Early diabetes feet
Diabetes feet in its early stages can have vague symptoms that are hard to recognize. It’s important to know all the signs of diabetes so you can act as soon as possible.
Early signs of diabetic feet in women and men
The earliest sign of diabetic feet is tingling, burning, numbness, and pain. But, these early signs can be hard to catch and might go unnoticed. Even mild symptoms of numbness and tingling may be signs that you have diabetes-related foot complications.
As someone living with type 1 diabetes myself, I examine my feet each morning. It take no more than about 20-30 seconds. Looking on the tops and bottoms of your feet for any new marks or feelings of numbness or tingling. Once I’ve looked over my feet, I give them a quick rub to make sure there’s not any new sensations or feelings happening when I apply pressure.
Your diabetes doctor may also recommend seeing a podiatrist regularly.
Early diabetes feet symptoms
Here are a list of common diabetes feet symptoms to be aware of and monitor for:
- Tingling feeling
- Numbness
- Burning sensation
- Weakness
- Pain in the legs and feet
- Change in temperature
- Change in color (red, blue, purple)
- Swelling
- Itching
- Slow healing wounds
- Open sores, cuts, red spots
- Dryness and cracked skin
- Unusual foot odor
Pictures of diabetic feet
Daily diabetes management should include examining the skin on your feet.
This article offers more in depth photos of diabetes feet symptoms. The CDC also has a helpful infographic featuring the different signs as well.
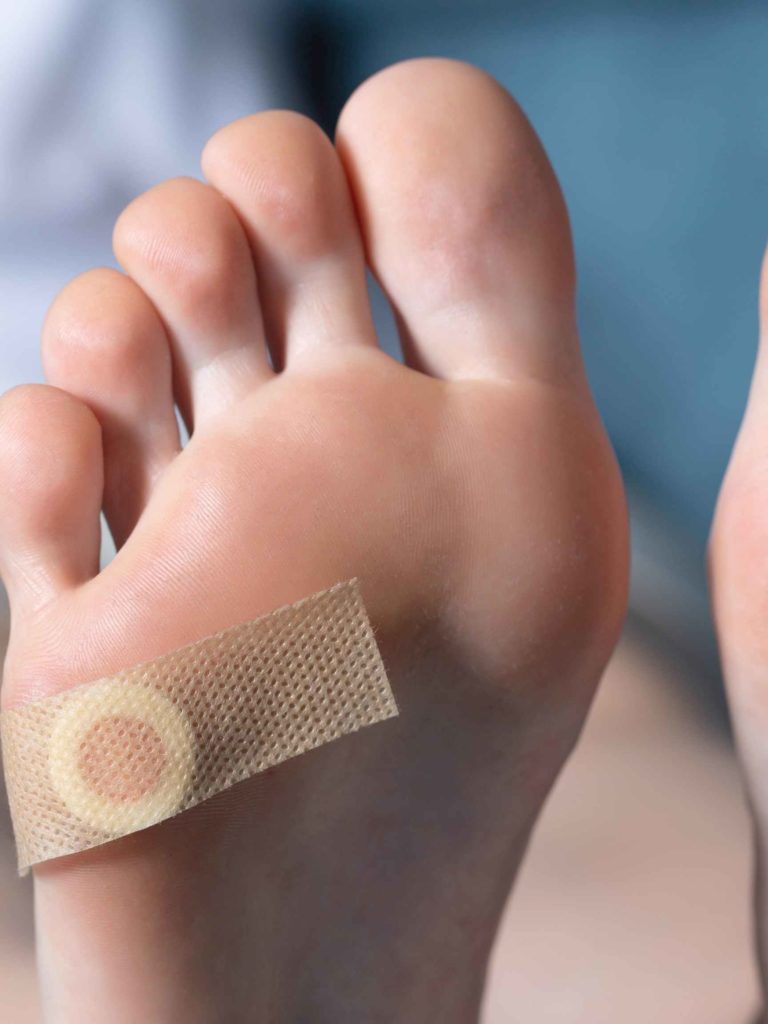
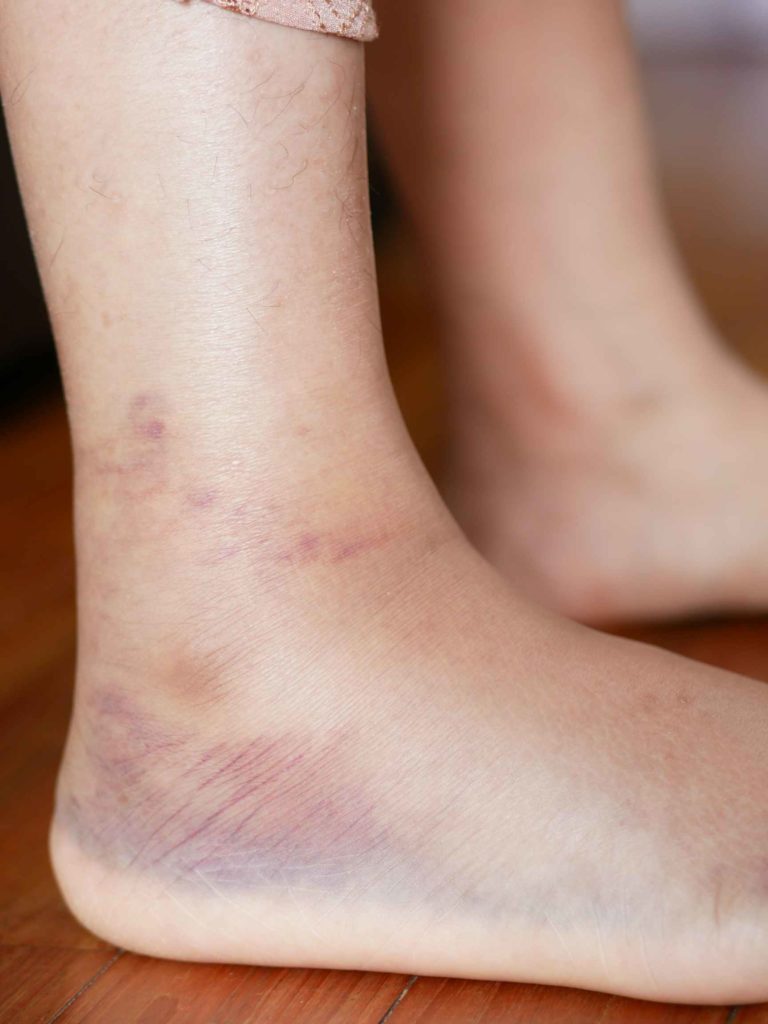
Diabetes and brown spots on feet
Brown spots on the skin are common for people with diabetes. It usually shows up on the shins, but can occur anywhere on the body, including the feet. Luckily, these spots aren’t harmful or painful. This condition is called “diabetic dermopathy.” These spots can occur from high blood sugars affecting blood vessels.
Diabetic neuropathy and feet
Neuropathy is the scientific term for nerve damage outside of our brain and spinal cord. In diabetes, high blood sugar over time can injure nerves so they aren’t able to work properly. Eventually, the nerve damage causes numbness. Usually, when we get a cut or a burn, our body tells the brain to send pain signals so we can know that something is wrong, Diabetic neuropathy makes it hard to send these signals and foot problems can go unnoticed and untreated.
Specific signs of diabetic neuropathy in feet:
- Tingling feeling
- Numbness
- Burning sensation
- Weakness
- Cramping
Diabetic nerve pain in feet
Diabetic neuropathy causes numbness, but it can also cause pain. It feels similar to when you move suddenly after your foot falls asleep and you feel a sharp, shooting feeling up your leg. This “shock” is pain caused by the nerve damage in feet.
Itchy feet and diabetes
Nerve damage in our feet can lead to dryness and itchy skin. While itchy skin itself isn’t harmful, when we scratch our feet often, it can lead to open sores and cuts without us realizing. This can cause more serious problems, like an infection.
I’ve dealt with periods of itchy feet myself over the years. To help, I like to apply lotion to the bottoms of the tops of my feet before going to bed and then cover my feet with socks to help retain some of the moisture from the lotion throughout the night.
Diabetic sores on feet
Diabetic sores on feet, or diabetic foot ulcers, are open sores that usually occur on the bottom of the foot. Foot ulcers can happen to anyone, but for people with diabetes, they may take longer to heal if blood sugars are not well managed. When the wound is open for too long or if it’s not treated properly, infections can happen. Out of all hospital admissions for diabetes complications, most result from diabetic foot ulcers.
Swollen feet and diabetes
High blood sugars not only damage nerves, but blood vessels too. Blood vessel injury leads to poor circulation that can cause swelling. On top of that, the nerve damage can make cuts, bruises, or sprains go unnoticed. These cause inflammation which also leads to swelling.
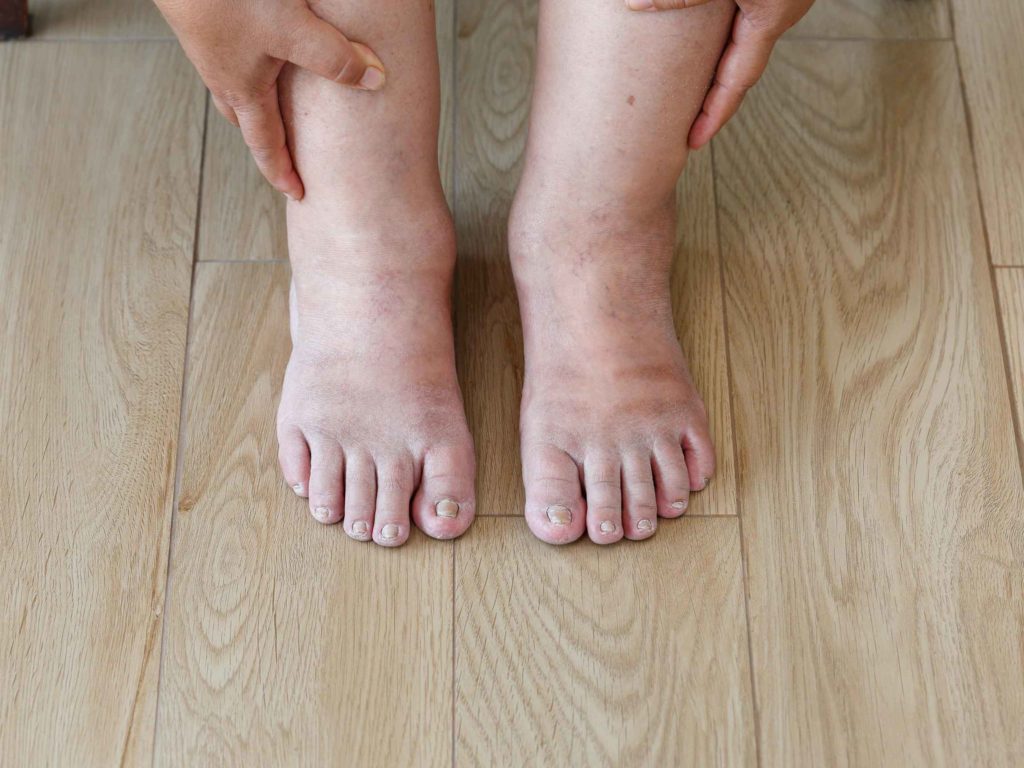
How do people with diabetes reduce swollen feet
Swollen feet aren’t just inconvenient, but they can be painful and uncomfortable. While you can’t fully avoid swollen feet from diabetes, here are some ways to help prevent them from happening.
- Elevate your feet when sitting
- Exercise and move your body throughout the day
- Wear compression socks
- Hydrate throughout the day
- Limit your salt intake
Elevate your feet when sitting
Put your feet above heart level while lying down to help swollen feet. If you can’t lie down fully, you can also use a small stool or foot rest to lift your feet slightly off the ground.
Exercise and move your body throughout the day
Regular exercise can increase blood flow. It also makes our cells more sensitive to insulin. It’s good practice to get 150 minutes of exercise every week for overall health.
Even if you can’t fit in a workout, moving your feet can help improve blood flow and lessen swelling. If you’re sitting for long periods of time, try walking for a few minutes every hour. You can also march in place if you can’t leave wherever you are.
Wear compression socks
Slight pressure from compression socks improves blood flow to the legs and feet. This can reduce swelling. But if it’s too tight, it can make the blood flow slower. If you wear compression socks, make sure they fit right for you. If you notice any numbness or discomfort from the socks, stop wearing them.
Hydrate throughout the day
Make sure you’re staying well hydrated. Sometimes when the body is dehydrated, it holds onto more water which can cause swelling.
Limit your salt intake
Similar to hydrating, too much salt causes our body to hold onto more water. This can make swelling worse. Choose more fresh foods, low-sodium products, and sodium-free herbs and spices.
Cold feet and diabetes
Humans are warm-blooded creatures because our blood keeps us, well, warm! To be more precise, it’s the way our body moves the blood in our body that keeps us warm. When blood vessels are damaged from diabetes, it’s hard for the body to send blood to these parts. This can lead to cold hands and feet.
Diabetic blisters on feet
The exact cause of blisters from diabetes isn’t fully understood, but they commonly occur due to poor fitting shoes and improper foot care. They can be small, around ½ inch in diameter, or up to 6 inches. While the blisters themselves aren’t harmful, popping them on your own can increase your risk of infection. If these blisters feel itchy, apply soothing anti-itch creams to the area.
Progression and outcomes of diabetes feet
Diabetes-related foot problems can start off mild. However, it is important to take even mild symptoms seriously. That’s because diabetes foot problems can progress quickly into more serious issues. Proper foot care is important to reduce the risk of infections, ulcers, and possible need for amputations. Luckily, these problems are preventable and treatable if you pay attention to your feet!
Actions to take for early diabetes feet
Follow these tips for keeping your feet healthy and safe while living with diabetes. Following these steps will help you detect any signs of early diabetes feet related problems.
- Check your feet daily for any changes
- Wash your feet daily
- Wear shoes that fit well
- Protect your feet
- Cur your toe nails straight across
- Don’t remove corns and calluses alone
- Enjoy regular movement/exercise
Check every day for early diabetes feet signs
Check your feet daily for any of the following:
- Cuts
- Redness
- Change of color
- Blisters
- Swelling
- Corns
- Calluses
- Infections
Going to the doctor every 3-6 months for a foot check isn’t enough. It’s important to check your feet every day so you can keep track of any changes in your feet. Don’t forget to check in between your toes and the bottom of your feet. You can use a mirror or ask someone to help you look at it closely if checking your feet is difficult.
Wash your feet every day
Use warm, soapy water to wash your feet. But make sure to dry them completely (especially between the toes) and to not leave them wet for too long. Apply lotion after you dry your feet to prevent dryness and cracking.
For more tips on diabetes skin care for dry skin, scars, and more, read this article.
Wear comfortable shoes that fit well
Make sure your shoes are pebble- and object-free and never go sock-less with closed-toe shoes. Choose shoes that fit comfortably and that don’t rub against the sides of your feet too much. When wearing new shoes, break them in slowly to avoid blisters.
Always protect your feet
Wear socks, slippers, or shoes inside and outside the home to protect your feet from injury.
Cut your toenails straight across
When you cut toenails at a curve, it can cause ingrown toenails to form. Make sure to file down the sharp corners after you cut the nail straight across.
If you choose to get pedicures, make sure you are going to a salon that practices good hygeine and uses sterile instruments. Ask your technician to cut your toe nails straight across as described above. Speak with your doctor about the risks of pedicures and if it’s ok for you to get one.
For myself, I will typically cut my own toe nails ahead of time to ensure they are cut in a way I am comfortable with. After speaking with my doctor, they were comfortable with me doing this part at home and then going to a salon for the other parts of a pedicure.
Don’t remove corns and calluses alone
Avoid using over-the-counter products to remove corns and calluses. Talk to your doctor about these problems.
Encourage movement
Wiggle your toes and put your feet up from time to time if you are sitting for long periods of time. This promotes blood flow to your feet.

Looking for more diabetes resources? Check out these other articles…





