
Traveling with diabetes can be very overwhelming, but it doesn’t have to be super scary.
One of the key things to managing diabetes well is staying consistent in your daily routines. And, when you’re traveling with diabetes, life is anything but consistent right?!
Can you travel with diabetes?
You should definitely chat with your doctor and other healthcare providers and get their recommendations and tips before traveling, but also make sure to keep reading for some not so common recommendations that you may not get on a handout from your doctor.
I’m giving you my tips after living (and traveling) with diabetes for almost 28 years… AND I’ve interviewed some of my favorite dietitians for their tips as well!
Tips for traveling with diabetes
Some recommendations when traveling with diabetes are quite common and you’ve likely heard them before… but others may be new to you. So, let’s dive in!
- Pack lots of snacks and bring extra low blood sugar treatments
- Wear a medical ID
- Stay hydrated
- Bring extra diabetes supplies and use ice packs and coolers
- Apply for TSA pre-check
- Bring an extra carryon bag for diabetes supplies when flying
- Pack diabetes supplies strategically
- Place insulin at the bottom of a hotel mini fridge
- Adjust insulin doses if changing time zones
- Know key diabetes phrases in the language of the country you are visiting
- Strive for consistency in your routine
1. Pack lots of snacks and bring extra low blood sugar treatments
Bring double the amount of low blood sugar treatments you think you’ll need. Some great travel friendly ideas for people traveling with diabetes include: dried fruit, honey packets, glucose gel, glucose tablets, and juice boxes.
“One thing I always tell people is to keep packets of gel icing or honey in their glovebox or carry-on incase they get stranded unexpectedly and have a low blood sugar. It’s something that stays good forever versus packing food that will spoil.” -Tabitha Odom, registered dietitian at OdomRD.com
2. Pack and wear your medical ID
This one goes without saying, but make sure there is a way for people to know you have diabetes if you are unable to communicate and get separated from the people you’re traveling with.
3. Stay hydrated while traveling with diabetes
Whether you’re flying on an airplane or just trying to prevent yourself from making too many stops on a road trip, we all tend to get dehydrated when we travel.
“Staying hydrated while traveling is important, especially when you have diabetes. Bring an empty reusable water bottle in your carryon and refill at the water fountain after airport security. Refill your water bottle during your trip and carry it with you while sightseeing. ” –Kylee Pedrosa, registered dietitian and diabetes coach at kyleepedrosanutrition.com
Need ideas for snacks and drinks to bring on a road trip? Check out Healthy Diabetes Snacks on the Go for Your Road Trip.
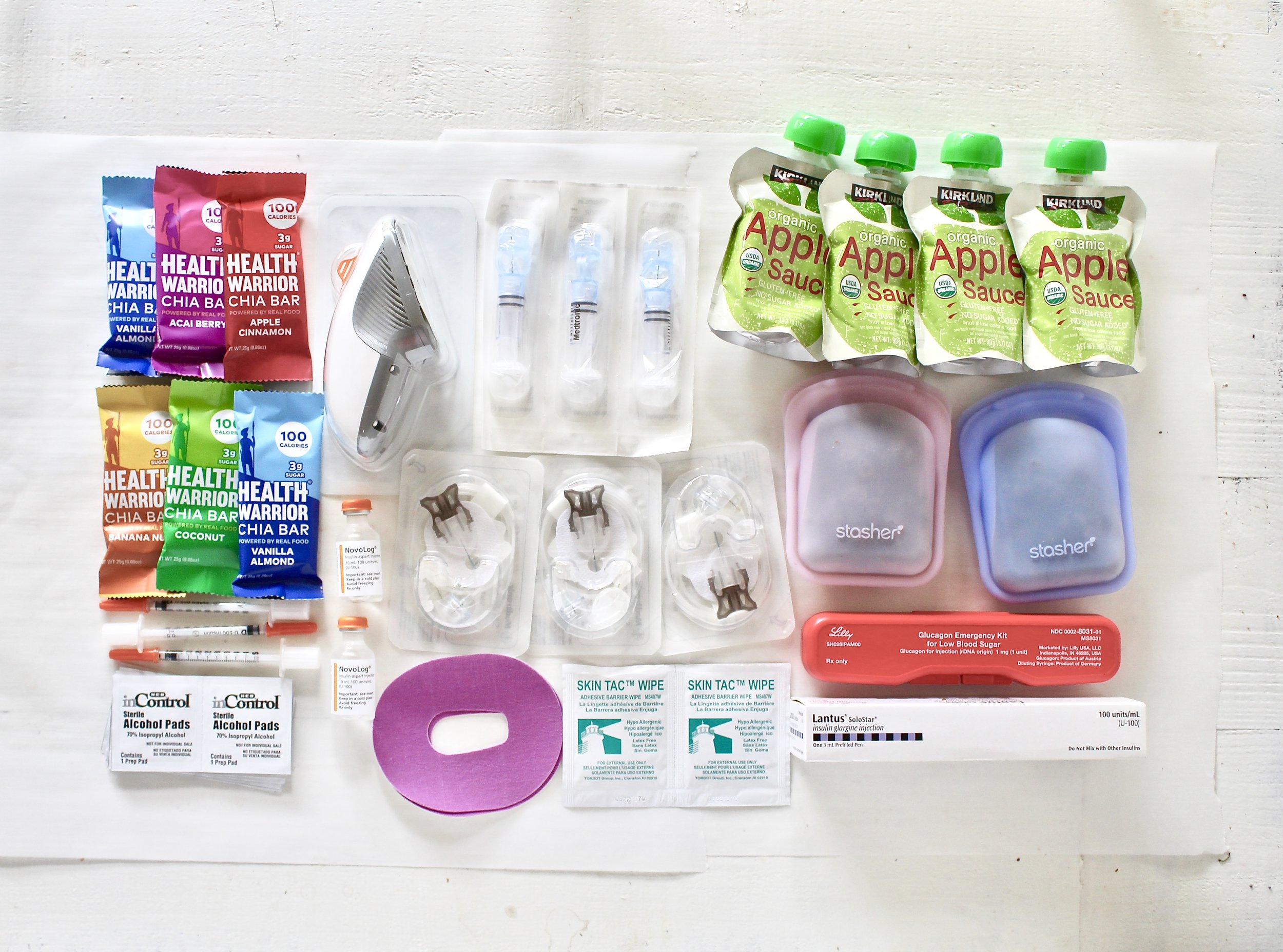
4. How to travel with diabetes supplies
Bring extras of EVERYTHING (test strips, CGM monitors, insulin, medications, pump supplies, lancets, syringes, etc.) I always advise people to plan as if you’re going to be gone for a week longer than you actually are. And while that most likely won’t happen, you never know what supplies might stop working or get lost.
Bring ice packs for medications if needed.
5. Apply for TSA pre-check if flying
Air travel in general can be stressful, especially with all the rules now around how many bags you can bring, etc. Apply for TSA Precheck if you are planning on flying. It makes getting through airport security with all your supplies so much easier.
Want to know more about going through airport security and flying with diabetes? Check out this post: Flying With Type 1 Diabetes: TSA & Insulin Tips.
6. Bring an extra carryon bag for diabetes supplies when flying
Most airlines allow you to bring an additional carryon for medical supplies (be sure to verify with your airline). Pack your supplies in a bag small enough to fit under the seat so there is no chance of your bag being checked due to limited overhead space.
“It’s always a good idea to remember to place your diabetes supplies in a carryon bag, NOT in your checked luggage.” –Jean LaMantia, registered dietitian at JeanLaMantia.com
Need tips for organizing your diabetes while traveling with diabetes or how to travel with diabetes needles? Check out Diabetes Supplies: Tips for Storage, Organization, and Travel.

7. Pack supplies strategically for long term traveling with diabetes
If you will be away for a long amount of time though, it may be important to take a different approach to packing your diabetes supplies. “I always recommend they divide supplies if possible between two carryon bags. I had a kid who did study abroad and all his supplies were in his backpack which got stolen. It was awful trying to get supplies and insulin to him.” –Sylvia White, registered dietitian and diabetes educator
8. Be careful using a hotel mini fridge
“It’s important to be careful when using the mini fridge at a hotel. Be careful about where you place the insulin in. I always put it towards the bottom instead of top because I’ve seen it freeze and ruin.” –Sylvia White, registered dietitian and diabetes educator
9. Adjust insulin doses if changing time zones when traveling with diabetes
“If changing time zones, be sure to adjust the timing of your insulin to avoid stacking or hypoglycemia. Might be a good idea to discuss with your doctor or diabetes educator ahead of time if the dose needs to be adjusted as you acclimate to a new time zone.” –Casey Seiden MS RD CDCES, registered dietitian and certified diabetes educator
10. International travel with diabetes: Know the language
If you’re traveling internationally or even just jumping over a few time zones, there are some additional things to consider. “Depending on where you are traveling….have a card written out in the language of the country you are visiting concerning info on you or your loved one’s diabetes.” – Susan E. Adams, registered dietitian and professor at LaSalle University
11. Strive for consistency in your routine
Travel often means a big change in routine, usually a good deal more or less activity and meals can often be larger as well. Both of these changes can cause large fluctuations in blood sugars.
“My biggest concern for my clients with diabetes (1 & 2) is the change of routine when someone is traveling… People are more prone to skip meals or go too long without eating and therefore eat larger meals, which can both cause fluctuations in blood sugar.
It is important to strategize with your dietitian/diabetes educator on a method for staying on a relatively consistent schedule. Maybe setting phone alarms, and “taking inventory of the day” to have a plan for accessible snacks in between meals. Find a way to fit some form of exercise in once a day – hotel gym, walking, etc. to help regulate blood sugar while out of the normal routine with potentially more larger meals.” – Chloe Paddison, registered dietitian at CureativeNutrition.com
Free traveling with diabetes checklist
Nervous about traveling with diabetes? I’ve got you covered. Download my free travel checklist to use next time you’re packing for a trip!

Do you have any tips of your own to share? Let me know in a comment!






4 Responses
These are great tips! We traveled a couple years ago and had the bomb squad called and my daughter patted down twice!!! Seriously! Her hands were clean, but after handling insulin regularly her bag with all her extra insulin/supplies was flagged as well. She has her bracelet on and the airport security were super gracious but they had to follow protocol.
The problem: insulin has glycerin in it, which is also a possible ingredient in a bomb. (The TSA schooled us). So if a drop has ever spilled there’s a possibility of traces of insulin (glycerin) as well. Once we were cleared and finally home, e took every thing out of the bag and wiped it down with Clorox wipes. She’s flown since then and not one incident.
All that to say, my mom tip, wipe down your bag(s) that hooks your insulin.
That’s a great tip! Thanks for sharing!
I have been flagged at the airport before too. The bomb residue test came up positive due to the perfume or lotion I was wearing. The TSA people said the scents can react from time to time. I am now very careful, since I know I usually have my hands swabbed since wearing an insulin pump, to not wear perfumed products when traveling.
Mary, this was so helpful. Staying active is a key strategy for diabetes management and there is no better way to do it than frequent travelling. Be careful of the altitude and temperature since these can impact your blood sugar levels. Do not forget your diabetic socks and medications for a fuss-free safe experience.